Disorders of bone mineral metabolism in patients with chronic kidney disease at the Hospital Nacional (2023-2024)
Main Article Content
Abstract
Introduction: alterations in bone mineral metabolism have an impact as a cardiovascular risk factor; it is necessary to recognize them early to prevent their progression. Objective: To describe the frequency of alterations in calcium-phosphorus metabolism in adult patients with chronic kidney disease (CKD) at different stages who attend the Hospital Nacional in the period 2023-2024.
Methodology: a descriptive, observational, cross-sectional, retrospective study that included adult patients with CKD at different stages. Demographic variables (sex, age, origin), laboratory variables (serum levels of PTH, calcium, vitamin D, and phosphorus), and clinical variables (CKD stage, presence of hypothyroidism, need for hemodialysis, comorbidities) were studied.
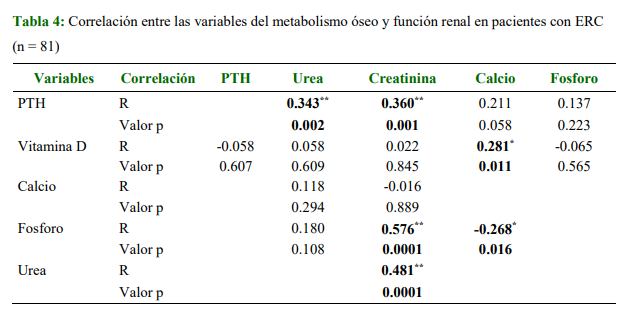
Results: 81 patients with CKD between 21 and 97 years of age (rIC:50,63)were included, 87 % from rural areas, 62 % (n = 50) male. Regarding comorbidities and etiologies of CKD, 52 % (n = 43) had type 2 diabetes mellitus, followed by arterial hypertension (13 %) among the most frequent. 86 % were in stage V, all on three-weekly dialysis. 85 % showed vitamin D deficiency. Hypothyroidism was found in 5 % (n = 4). An association was observed between higher levels of phosphate and lower levels of calcium in advanced stages of the disease and an increase in PTH from stage IV showing an association with higher levels of urea and creatinine.
Conclusion: a high frequency of alterations in bone mineral metabolism was found from early stages of the disease, therefore its routine study should be a common practice in order to provide adequate supplementation and avoid progression to secondary hyperparathyroidism
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
References
Fernández LM, Sánchez-Alvarez JE, Morís de la Tassa C, Bande Fernández JJ, María V, Fernández E, et al. Risk factors associated with valvular calcification in patients with chronic kidney disease. Analysis of NEFRONA Study. Nefrologia [Internet]. 2021;41(3):337-346. doi: 10.1016/j.nefro.2020.08.012.
Bover J, Ureña P, Torregrosa JV, Rodríguez-García M, Castro-Alonso C, Górriz JL, et al. Osteoporosis, densidad mineral ósea y complejo CKD-MBD (I): consideraciones diagnósticas [Internet]. Nefrología. 2018;38(2):476-490. doi: 10.1016/j.nefro.2017.12.006
Hsu HJ, Wu IW, Hsu KH. Chiao-Yin S, Chun-Yu Ch, Chin-Chan L. Vitamin D deficiency, cardiothoracic ratio, and long-term mortality in hemodialysis patients. Scientific Reports [Internet]. 2020;10:7533. doi: 10.1038/s41598-020-64359-9
Dawson-Hughes B, Mithal A, Bonjour JP, Boonen S, Burckhardt P, Fuleihan GE, et al. IOF position statement: vitamin D recommendations for older adults. Osteoporos Int. 2010;21(7):1151.
Torregrosa JV, Bover J, Rodríguez Portillo M, González Parra E, Arenas MD, et al. Recommendations of the Spanish Society of Nephrology for the management of mineral and bone metabolism disorders in patients with chronic kidney disease: 2021 (SEN-MM). Nefrologia.
;42(Supp 3): 1-37. doi: 10.1016/j.nefro.2022.03.007
Delgado Lombardi N, Cazo M. Alteraciones del metabolismo óseo mineral en pacientes hemodializados en el Hospital Nacional de Itauguá. Rev. Soc. Parag. Nefrol. [Internet]. [citado 6 de septiembre de 2024];2023;1(1):10-7. doi: 10.70108/nefrologiapy.2023.1.1.10
Lujan Ramos MA, Ramírez Arce JA, Acevedo Romero JM, Gómez Jiménez S, Cañas Osorio JM, Santander Bohorquez D, et al. Vasculitis en adultos mayores. Prevalencia de las alteraciones del metabolismo óseo-mineral asociadas a enfermedad renal crónica no en diálisis. Rev. Colomb.
Nefrol. 2019;6(1):17-27. doi: 10.22265/acnef.6.1.311.
Bruzzone ME, Giammona AM, Touceda L, Onofri F, Genchi C, Del Amo M. Calcificaciones vasculares y valvulares en pacientes en hemodiálisis crónica. Rev. nefrol. dial. traspl. [Internet]. 2014 [citado 2024 Sep 06]; 34(4):183-190. Disponible en: https://www.scielo.org.ar/pdf/nefro/v34n4/v34n4a03.pdf
National Kidney Foundation. K/ DOQI clinical practice guidelines for bone metabolism and disease in chronic kidney disease. Am J Kidney Dis. 2003;42(4 Suppl 3):S1-201.
Kidney Disease: Improving Global Outcomes (KDIGO) CKD-MBD Update Work Group. KDIGO 2017 clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD). Kidney Int Suppl (2011). 2017;7(1):1-59. doi: 10.1016/j.kisu.2017.04.001
Cupisti A, Vigo V, Baronti ME, DÁlessandro C, Ghiadoni L, Egidi MF. Vitamin D status and cholecalciferol supplementation in chronic kidney disease patients: an Italian cohort report. Int J Nephrol Renovasc Dis. 2015;8: 151–7. doi: 10.2147/IJNRD.S90968
Junyu Z, Jianjun D, Haipeng W, Hongxia S, Dongmei Z, Lin L. Efficacy and safety of vitamin D3 in patients with diabetic nephropathy: a meta-analysis of randomized controlled trials. Chin Med J (Engl). 2014;127(15): 2837-43. https://pubmed.ncbi.nlm.nih.gov/25146624/
Kramer H, Berns JS, Choi MJ, Martin K, Rocco MV. 25-Hydroxyvitamin D testing and supplementation in CKD: an NKF-KDOQI controversies report. Am J KidneyDis. 2014;64(4): 499–509. doi: 10.1053/j.ajkd.2014.05.018
Restrepo Valencia CA, Aguirre Arango JV. Vitamin D (25(OH)D) in patients with chronic kidney disease stages 2-5. Colomb Med (Cali). 2016;47(3):160-166.
Baraia-Etxaburu-Astigarraga M, Baraia-Etxaburu-Artetxe JM. Estudio de los niveles de vitamina D en diversas poblaciones. Gac Med Bilbao. 2017;114(3):97-106. https://www.gacetamedicabilbao.eus/index.php/gacetamedicabilbao/article/view/259/265
Yeung WG, Toussaint ND, Badve SV. Vitamin D therapy in chronic kidney disease: a critical appraisal of clinical trial evidence. Clin Kidney J. 2024;17(8):sfae227. doi: 10.1093/ckj/sfae227.
Zaimi M, Grapsa E. Current therapeutic approach of chronic kidney disease-mineral and bone disorder. Ther Apher Dial. 2024;28(5):671-689. doi: 10.1111/1744-9987.14177.
Ennis JL, Worcester EM, Coe FL, Sprague SM. Current recommended 25-hydroxyvitamin D targets for chronic kidney disease management may be too low. J Nephrol. 2016;29(1):63-70. doi: 10.1007/s40620-015-0186-0.