Aceptabilidad del PrEP en hombres que tienen sexo con hombres (HSH) revisión sistemática de estudios cualitativos
Contenido principal del artículo
Resumen
Objetivo: analizar los estudios que indaguen la aceptabilidad del PrEP en Hombres que tienen sexo con Hombres (HSH).
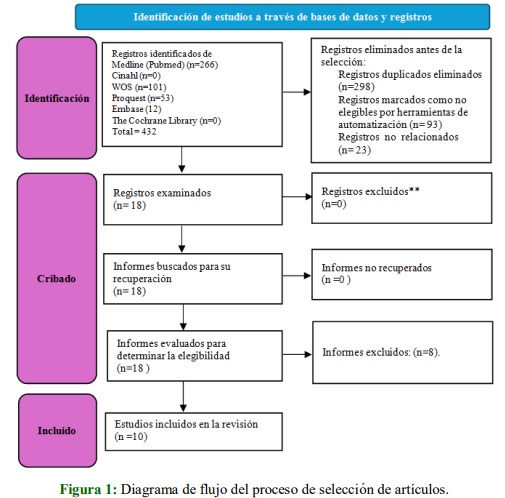
Metodología: se realizó una búsqueda sistemática de estudios publicados en inglés o castellano, hasta junio de 2024, que indagaran en las Aceptabilidad del PrEP en HSH. La búsqueda se realizó en las siguientes bases de datos electrónicas: The Cochrane Library, Medline (Pubmed), PsycINFO, EMBASE, Web of Science, y CINHAL.
Resultados: tras la búsqueda en las bases de datos analizadas se encontraron 432 articulos. Los participantes reportaron beneficios como la reducción de la ansiedad relacionada con el VIH, mejor participación en la atención médica y mayor comodidad sexual. Sin embargo, también se identificaron barreras significativas, incluyendo el estigma, preocupaciones sobre efectos secundarios, problemas de adherencia, y desafíos relacionados con el costo y acceso.
Conclusiones: esta revisión cualitativa proporciona una comprensión matizada y multifacética de las experiencias, percepciones y desafíos relacionados con el PrEPentre diversas poblaciones de HSH.
Detalles del artículo

Esta obra está bajo una licencia internacional Creative Commons Atribución 4.0.
Usted es libre de:
- Compartir: copiar y redistribuir el material en cualquier medio o formato para cualquier propósito, incluso comercialmente.
- Adaptar: remezclar, transformar y construir a partir del material para cualquier propósito, incluso comercialmente.
- La licenciante no puede revocar estas libertades en tanto usted siga los términos de la licencia
Bajo los siguientes términos:
- Atribución: Usted debe dar crédito de manera adecuada, brindar un enlace a la licencia, e indicar si se han realizado cambios. Puede hacerlo en cualquier forma razonable, pero no de forma tal que sugiera que usted o su uso tienen el apoyo de la licenciante.
- Compartir igual: — Si remezcla, transforma o crea a partir del material, debe distribuir su contribución bajo la misma licencia del original.
- No hay restricciones adicionales — No puede aplicar términos legales ni medidas tecnológicas que restrinjan legalmente a otras a hacer cualquier uso permitido por la licencia.
Citas
Grant RM, Lama JR, Anderson PL, McMahan V, Liu AY, Vargas L, et al. Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med. 2010;363(27):2587-99. doi: 10.1056/NEJMoa1011205.
Molina JM, Capitant C, Spire B, Pialoux G, Cotte L, Charreau I, et al. On-Demand preexposure prophylaxis in men at high risk for HIV-1 infection. N Engl J Med. 2015;373(23):2237-46. doi: 10.1056/NEJMoa1506273.
Mayer KH, Hosek S, Cohen S, Liu A, Pickett J, Warren M, et al. Antiretroviral pre-exposure prophylaxis implementation in the United States: a work in progress. J Int AIDS Soc. 2015;18(4 Suppl 3):19980. doi: 10.7448/IAS.18.4.19980.
Nair G, Celum C, Szydlo D, Brown ER, Akello CA, Nakalega R, et al. Adherence, safety, and choice of the monthly dapivirine vaginal ring or oral emtricitabine plus tenofovir disoproxil fumarate for HIV pre-exposure prophylaxis among African adolescent girls and young women: a randomised, open-label, crossover trial. Lancet HIV. 2023;10(12):e779-e789. doi: 10.1016/S2352-3018(23)00227-8.
Koechlin FM, Fonner VA, Dalglish SL, O'Reilly KR, Baggaley R, Grant RM, et al. Values and preferences on the use of oral pre-exposure prophylaxis (PrEP) for HIV prevention among multiple populations: a systematic review of the literature. AIDS Behav. 2017;21(5):1325-1335. doi: 10.1007/s10461-016-1627-z.
Sullivan PS, Carballo-Diéguez A, Coates T, Goodreau SM, McGowan I, Sanders EJ, et al. Successes and challenges of HIV prevention in men who have sex with men. Lancet. 2012;380(9839):388-99. doi: 10.1016/S0140-6736(12)60955-6.
Kirby T, Thornber-Dunwell M. Uptake of PrEP for HIV slow among MSM. Lancet. 2014;383(9915):399-400. doi: 10.1016/s0140-6736(14)60137-9.
Golub SA, Gamarel KE, Rendina HJ, Surace A, Lelutiu-Weinberger CL. From efficacy to effectiveness: facilitators and barriers to PrEP acceptability and motivations for adherence among MSM and transgender women in New York City. AIDS Patient Care STDS. 2013;27(4):248-54. doi: 10.1089/apc.2012.0419.
Calabrese SK, Underhill K. How stigma surrounding the use of HIV preexposure prophylaxis undermines prevention and pleasure: a call to destigmatize "Truvada Whores". Am J Public Health. 2015;105(10):1960-4. doi: 10.2105/AJPH.2015.302816.
Gomez GB, Borquez A, Case KK, Wheelock A, Vassall A, Hankins C. The cost and impact of scaling up pre-exposure prophylaxis for HIV prevention: a systematic review of cost-effectiveness modelling studies. PLoS Med. 2013;10(3):e1001401. doi: 10.1371/journal.pmed.1001401.
Eaton LA, Matthews DD, Driffin DD, Bukowski L, Wilson PA, Stall RD; POWER Study Team. A multi-us city assessment of awareness and uptake of pre-exposure prophylaxis (PrEP) for HIV prevention among black men and transgender women who have sex with men. Prev Sci. 2017;18(5):505-516. doi: 10.1007/s11121-017-0756-6.
Sullivan PS, Mena L, Elopre L, Siegler AJ. Implementation strategies to increase PrEP uptake in the south. Curr HIV/AIDS Rep. 2019;16(4):259-269. doi: 10.1007/s11904-019-00447-4.
Nunn AS, Brinkley-Rubinstein L, Oldenburg CE, Mayer KH, Mimiaga M, Patel R, et al. Defining the HIV pre-exposure prophylaxis care continuum. AIDS. 2017;31(5):731-734. doi: 10.1097/QAD.0000000000001385.
Tong A, Flemming K, McInnes E, Oliver S, Craig J. Enhancing transparency in reporting the synthesis of qualitative research: ENTREQ. BMC Med Res Methodol. 2012;12:181. doi: 10.1186/1471-2288-12-181.
Olmo RS. Programa de habilidades en lectura crítica español (CASPe). NefroPlus. 2017: 9(1):100-101.
Zapata JP, Petroll AE, de St. Aubin E, Quinn K. Perspectives on social support and stigma in PrEP-related care among gay and bisexual men: a qualitative investigation. J Homosex. 2020;67(11):1582-1607.
Owens C, Hubach RD, Williams D, Lester J, Reece M, Dodge B. Exploring the pre-exposure prophylaxis (PrEP) health care experiences among men who have sex with men (MSM) who live in rural areas of the midwest. AIDS Educ Prev. 2020;32(1):51-66. doi: 10.1521/aeap.2020.32.1.51.
Dubov A, Galbo P Jr, Altice FL, Fraenkel L. Stigma and shame experiences by MSM who take PrEP for HIV prevention: a qualitative study. Am J Mens Health. 2018;12(6):1843-1854.
Peters RMAH, van der Loeff MFS, Prins M. Sexual risk behaviour and STI testing among MSM engaging in paid sex work in the Netherlands: a qualitative study. Sex Transm Infect. 2023;99(1):39-44.
Nguyen LH, Nguyen HLT, Tran BX, Larsson M, Rocha LEC, Thorson A, Strömdahl S. A qualitative assessment in acceptability and barriers to use pre-exposure prophylaxis (PrEP) among men who have sex with men: implications for service delivery in Vietnam. BMC Infect Dis.
;21(1):472. doi: 10.1186/s12879-021-06178-5.
Wong NS, Kwan TH, Lee KCK. Investigating the attitudes of men who have sex with men towards HIV pre-exposure prophylaxis use in Hong Kong: a qualitative study. Sex Health. 2019;16(3):233-239.
Patel RR, Crane JS, Rothwell E. Qualitative study of the acceptability of long-acting injectable pre-exposure prophylaxis among young Black men who have sex with men in the United States. AIDS Care. 2018;30(11):1385-1390.
Storholm ED, Volk JE, Marcus JL. Risk perception, sexual behaviors, and PrEP adherence among substance-using men who have sex with men: a qualitative study. Prev Sci. 2017;18(6):737-747.
Viera A, Cassels S, Patel RR. "I need to know more": a qualitative exploration of the PrEP knowledge, attitudes, and informational needs of Black and Latino men who have sex with men and use stimulants. AIDS Educ Prev. 2022;34(2):95-112.
Quinn KG, Christenson E, Spector A. The unanticipated benefits of PrEP for young black gay, bisexual, and other men who have sex with men. AIDS Behav. 2020;24(5):1376-1388.
García M, Harris AL. PrEP awareness and decision-making for Latino MSM in San Antonio, Texas. PLoS One. 2017;12(9):e0184014. doi: 10.1371/journal.pone.0184014.
Gyamerah AO, Kinzer E, Aidoo-Frimpong G, Sorensen G, Mensah MD, Taylor KD, et al. PrEP knowledge, acceptability, and implementation in Ghana: perspectives of HIV service providers and MSM, trans women, and gender diverse individuals living with HIV. PLOS Glob Public Health. 2023;3(6):e0001956. doi: 10.1371/journal.pgph.0001956.
Liu Y, Liu X, Wei S, Cheng Z, Xian Y, Zhao Y, et al. Identifying patterns of sexual behaviors and PrEP uptake characteristics among MSM who were eligible for PrEP: a national cross-section study. J Virus Erad. 2024;10(2):100382. doi: 10.1016/j.jve.2024.100382.
Stansfield SE, Heitner J, Mitchell KM, Doyle CM, Milwid RM, Moore M, et al. Populationlevel impact of expanding PrEP coverage by offering long-acting injectable PrEP to MSM in three high-resource settings: a model comparison analysis. J Int AIDS Soc. 2023;26 Suppl 2(Suppl 2):e26109. doi: 10.1002/jia2.26109.
Wahome E, Graham S, Thiong'o A, Chirro O, Mohamed K, Gichuru E, et al. Assessment of PrEP eligibility and uptake among at-risk MSM participating in a HIV-1 vaccine feasibility cohort in coastal Kenya. Wellcome Open Res. 2020;4:138. doi: 10.12688/wellcomeopenres.15427.2.
Manguro GO, Musau AM, Were DK, Tengah S, Wakhutu B, Reed J, et al. Increased condom use among key populations using oral PrEP in Kenya: results from large scale programmatic surveillance. BMC Public Health. 2022;22(1):304. doi: 10.1186/s12889-022-12639-6.
Mitchell KM, Boily MC, Hanscom B, Moore M, Todd J, Paz-Bailey G, et al. Estimating the impact of HIV PrEP regimens containing long-acting injectable cabotegravir or daily oral tenofovir disoproxil fumarate/emtricitabine among men who have sex with men in the United States: a
mathematical modelling study for HPTN 083. Lancet Reg Health Am. 2023;18:100416. doi: 10.1016/j.lana.2022.100416.