Skin infections: clinical and microbiological characteristics in a fourth level hospital
Main Article Content
Abstract
Introduction: skin and soft tissue infections are a common cause of medical consultations. The growing resistance to Staphylococcus aureus represents a significant therapeutic challenge.
Objective: to describe the clinical and microbiological characteristics in patients with skin and soft tissue infections admitted to the Hospital Nacional during 2024.
Methodology: a descriptive, analytical, retrospective, cross-sectional observational study was conducted using data from clinical records.
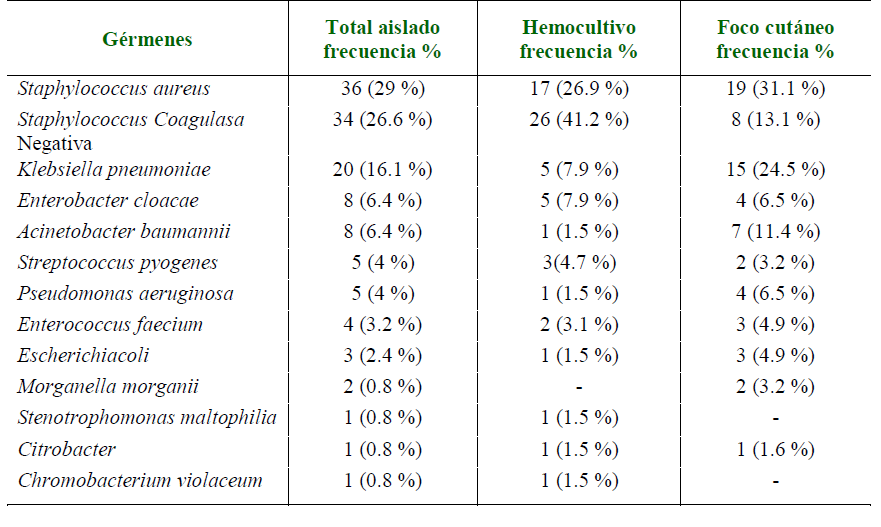
Results: 224 medical records were evaluated, with a diagnosis of skin and soft tissue infection. Males predominated in 71 %. The mean age was 54±16 years. The most frequent comorbidity was high blood pressure (48 %). Cellulitis was the most frequent skin and soft tissue infection (63 %). Isolations from cutaneous sources and blood cultures were 66 % and 47 %, respectively. The most frequently isolated germs were Staphylococcus aureus (29 %), coagulase-negative Staphylococcus (26.6 %), and Klebsiella pneumoniae (16.1 %). S. aureus showed a resistance of (58 %) to oxacillin and erythromycin (52 %). Sepsis occurred in 7 % of cases and was associated with older age, female sex, type 2 diabetes mellitus, and chronic kidney disease. Mortality was 9 % with a strong
association with sepsis.
Conclusions: SSTIs mostly affect men; however, in this series, female gender was associated with higher mortality. The high resistance of S. aureus to oxacillin emphasizes the need to update empirical treatment protocols in Paraguay.
Article Details

This work is licensed under a Creative Commons Attribution 4.0 International License.
Usted es libre de:
- Compartir: copiar y redistribuir el material en cualquier medio o formato para cualquier propósito, incluso comercialmente.
- Adaptar: remezclar, transformar y construir a partir del material para cualquier propósito, incluso comercialmente.
- La licenciante no puede revocar estas libertades en tanto usted siga los términos de la licencia
Bajo los siguientes términos:
- Atribución: Usted debe dar crédito de manera adecuada, brindar un enlace a la licencia, e indicar si se han realizado cambios. Puede hacerlo en cualquier forma razonable, pero no de forma tal que sugiera que usted o su uso tienen el apoyo de la licenciante.
- Compartir igual: — Si remezcla, transforma o crea a partir del material, debe distribuir su contribución bajo la misma licencia del original.
- No hay restricciones adicionales — No puede aplicar términos legales ni medidas tecnológicas que restrinjan legalmente a otras a hacer cualquier uso permitido por la licencia.
References
Stevens DL, Bisno AL, Chambers HF, Dellinger EP, Goldstein EJ, Gorbach SL, et al. Practice guidelines for the diagnosis and management of skin and soft tissue infections. Clin Infect Dis. 2014;59(2):147–59.doi: 10.1093/cid/ciu444.
Ki V, Rotstein C. Bacterial skin and soft tissue infections in adults: a review of their epidemiology, pathogenesis, diagnosis, treatment and site of care. Can J Infect Dis Med Microbiol. 2008;19(2):173–84.doi: 10.1155/2008/846453.
May AK. Skin and soft tissue infections: the new surgical infection society guidelines. Surg Infect (Larchmt). 2011;12(3):179–84.doi: 10.1089/sur.2011.034.
Miller LG, Eisenberg DF, Liu H, Chang CL, Wang Y, Luthra R, et al. Incidence of skin and soft tissue infections in ambulatory and inpatient settings, 2005-2010. BMC Infect Dis. 2015;15:362. doi: 10.1186/s12879-015-1071-0.
Dryden MS. Complicated skin and soft tissue infection. J Antimicrob Chemother. 2010;65 Suppl3:iii35–44. doi: 10.1093/jac/dkq302.
Stevens DL, Bryant AE. Necrotizingsoft-tissue infections. N Engl J Med. 2017;377(23):2253–65. doi: 10.1056/NEJMra1600673
Lipsky BA, Dryden M, Gottrup F. Antimicrobial stewardship in wound care: a position paper from the british society for antimicrobial chemotherapy and european wound management association. J Antimicrob Chemother. 2016;71(11):3026–35.doi: 10.1093/jac/dkw287.
Eron LJ, Lipsky BA, Low DE, Nathwani D, Tice AD, Volturo GA. Managing skin and soft tissue infections: expert panel recommendations on key decision points. J Antimicrob Chemother. 2003;52(Suppl 1):i3–17. doi: 10.1093/jac/dkg466.
Anaya DA, Dellinger EP. Necrotizing soft-tissue infection: diagnosis and management. Clin Infect Dis. 2007;44(5):705–10. doi: 10.1086/511638.
Ray GT, Suaya JA, Baxter R. Incidence, microbiology, and patient characteristics of skin and soft-tissue infections in a U.S. population: a retrospective population-based study. BMC InfectDis. 2013;13:252. doi: 10.1186/1471-2334-13-252.
Asenjo A, Oteo-Iglesias J, Alós JI. What’s new in mechanisms of antibiotic resistance in bacteria of clinical origin? Enferm Infecc Microbiol Clin (Engl Ed). 2021;39(6):291-9.doi: 10.1016/j.eimce.2020.02.017.
Paraguay. Ministerio de Salud Pública y Bienestar Social. RAM: conozca más sobre la resistencia antimicrobiana [Internet]. Asunción: MSPBS; 2025 [citado 19 ago 2025]. Disponible en: https://www.mspbs.gov.py/portal/26480/ram-conozca-mas-sobre-la-resistencia-antimicrobiana.html
World Health Organization. Antibiotic resistance [Internet].Geneva: WHO; 2025 [citado 19 ago 2025]. Disponible en: https://www.who.int/es/news-room/fact-sheets/detail/antibiotic-resistance
Justine BN, Mushi MF, Silago V, Igembe Z, Muyombe J, Kishengena PP, et al. Antimicrobial resistance surveillance of skin and soft tissue infections: hospital-wide bacterial species and antibiograms to inform management at a zonal tertiary hospital in Mwanza, Tanzania. Infect Drug
Resist. 2025;18:791-802. doi: 10.2147/IDR.S483953
Ruiz AJL, Nasr HAH, Zerpa H. Infecciones de piel y partes blandas en pacientes del servicio de traumatología. Rev Conecta Lib. 2020;4(3):1-14.
Giménez Ortigoza VD, Torres PR. Diabetes en pacientes con infección de piel y partes blandas internados en el Hospital de Clínicas. Rev Investig Cient Tecnol. 2020;4(2):49–57. doi:10.36003/Rev.investig.cient.tecnol.V4N2(2020)5
Linz MS, Mattappallil A, Finkel D, Parker D. Clinical impact of Staphylococcus aureus skin and soft tissue infections. Antibiotics (Basel). 2023;12(3):557. doi: 10.3390/antibiotics12030557.
Monk EJM, Jones TPW, Bongomin F, Kibone W, Nsubuga Y, Ssewante N, et al. Antimicrobial resistance in bacterial wound, skin, soft tissue and surgical site infections in Central, Eastern, Southern and Western Africa: a systematic review and meta-analysis. PLOS Glob Public Health. 2024;4(4):e0003077. doi: 10.1371/journal.pgph.0003077.
Natsis NE, Cohen PR. Coagulase-negative Staphylococcus skin and soft tissue infections. Am J Clin Dermatol. 2018;19(5):671-7. doi: 10.1007/s40257-018-0362-9.
Wu M, Guo F, He X, Zheng D, Ye W, Li S, et al. Analysis of distribution and drug susceptibility test results of pathogenic bacteria in diabetic foot ulcers. Diabetes Ther. 2024;15(7):1627-37. doi: 10.1007/s13300-024-01601-x.
Collazos J, de la Fuente B, de la Fuente J, García A, Gómez H, Menéndez C, et al. Factors associated with sepsis development in 606 Spanish adult patients with cellulitis. BMC Infect Dis. 2020;20(1):211. doi: 10.1186/s12879-020-4915-1.
Ogica A, Burdelski C, Rohde H, Kluge S, de Heer G. Necrotizing soft tissue infections in intensive care. J Intensive Care Med. 2022;37(3):393-400. doi: 10.1177/08850666211010127
Algethamy HM, Alhazmi RN, Alghalayini FK, Bahowarth SY, Bukhari NM, Alnosani LB, et al. Predictors of sepsis, intensive care unit admission, and death in patients hospitalized for complicated skin and soft tissue infections: retrospective study at a large tertiary-care center. SAGE
Open Med. 2025;13:20503121251336069. doi: 10.1177/20503121251336069.
Kim EJ, Ha KH, Kim DJ, Choi YH. Diabetes and the risk of infection: a national cohort study. Diabetes Metab J. 2019;43(6):804-14. doi: 10.4093/dmj.2019.0071.
Westgeest AC, Lambregts MMC, Ruffin F, Korn RE, Webster ME, Kair JL, et al. Female sex and mortality in patients with Staphylococcus aureus bacteremia.JAMA Netw Open. 2024;7(2):e240473. doi: 10.1001/jamanetworkopen.2024.0473.
Eachempati SR, Hydo L, Barie PS. Gender-based differences in outcome in patients with sepsis. Arch Surg. 1999;134(12):1342-7. doi: 10.1001/archsurg.134.12.1342.